News
Natalie Holborow
Nov 14, 2016

Natalie Holborow
You don’t forget being diagnosed with diabetes, no matter how young you were, or how little you understood about it at the time.
It was December, and where I should have been excited for Christmas, I instead found myself bony and awkward on a starched white bed with a drip in my hand and my father stroking my hair.
Every time a hand appeared on the curtain, I would ball up to the pillow and curl my hands in, terrified it was another injection.
I didn’t realise then it was the start of a future of life as a Type 1 diabetic.
I don’t think much of it now, sliding a cannula into my stomach and wearing an insulin pump attached to the waistband of my jeans. It doesn’t chill me, seeing a tiny red globe of scarlet gleaming on my fingertip. Before I went onto insulin pump treatment, it was the norm to slip a 4mm needle into my thigh 3-5 times a day.
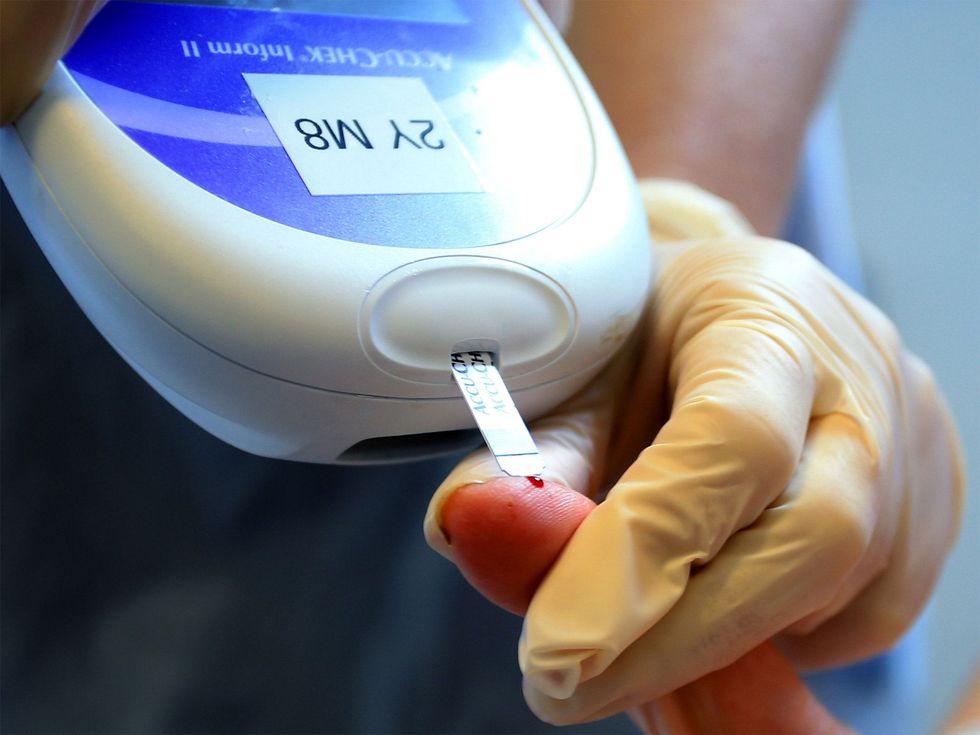
Everything revolves around numbers: grams of carbohydrates, blood glucose readings, insulin units.
Though diabetes is becoming more and more common, it is often Type 2, or diet-controlled diabetes, that is focused on in the media, leading to a lot of misconceptions.
Common questions include:
● ‘Should you be eating that?’
● ‘So how are you able to exercise?’
● ‘You can’t eat sugar, right?’
● ‘If you collapse, do I give you insulin?’
And, possibly worst of all, is being excluded in staff rooms when the biscuit tin is passed around, with an awkward smile and the assumption that:
● ‘I’d offer you one, but you can’t eat these.’
Though it’s important for anyone to eat healthily, so long as I calculate the amount of carbohydrates for what I’m going to eat, there is no reason why I can’t share a slice of birthday cake with you, or have popcorn at the cinema, or treat myself to a dessert, and it’s these enduring misconceptions and lack of distinction between the different types of diabetes that often leads to awkward situations.Whilst Type 1 and Type 2 diabetes are very different conditions, there is no diabetes which is ‘more serious’ than the other – they’re just managed differently.
Whilst diabetes is characterised by having higher than normal blood sugar levels, the cause and development of the conditions are different. Type 1 diabetes is an autoimmune disease where the pancreas becomes incapable of producing insulin. As a result, treatment always involves insulin, either via injections or insulin pump. There is no known cause for Type 1 diabetes, and it tends to occur much earlier in life. Type 2 diabetes is the most common form of diabetes, affecting 90% of the UK population at some point, and is caused by insulin resistance, sometimes as a result of lifestyle. According to JDRF, Type 2 can usually be managed through diet, exercise, and self-monitoring blood glucose, at least in the first few years following diagnosis. However, type 2 diabetes is a progressive condition, and most people will need to take tablets and/or inject insulin after living with it for five to 10 years.
Other forms of diabetes include:
● Gestational diabetes
● Maturity onset diabetes of the young (MODY)
● Neonatal diabetes
● Wolfram Syndrome
● Alström Syndrome
Though living with the condition can feel like a lot of extra responsibility, and I often find myself frustrated or lacking energy depending on my blood sugar readings (these have a huge impact on mood too), it doesn’t have to stop you achieving things so long as you’re prepared to put in the extra work. Last year, I completed my third half-marathon and have signed up to do the full Edinburgh Marathon for charity next May.
This I know will be challenging in terms of managing insulin doses and maintaining my blood glucose levels for extended periods of exercise – where I’m most likely to suffer a hypoglycaemic (low blood sugar) attack – but I’m lucky to have a great team of diabetes specialists who have always helped me when I’ve needed them. There’s been a lot of trial and error, and there are plenty of mistakes along the way, but I’ve recently accepted that as part of life with diabetes, and feel stronger and more at peace with myself for doing so.
If I could say anything to another person with diabetes, it would be to never say no to something because of the fear that diabetes will stop you. Though it may feel that way sometimes, it doesn’t have to own you. While we can’t ever do the job of an actual pancreas, we can only do our best with our diabetes treatment, and you absolutely should go out with your friends on a Friday night, or apply for that dream job, or do that triathlon, or go on that long-haul holiday. After all the carb-counting, you probably need it!
And to those who perhaps don’t quite understand what it means to live with diabetes, I want to say that it’s perfectly okay to ask questions.
It’s okay to approach me and question why I test my blood, or why there’s something attached to my hip. I’d be far happier to explain to you what I’m doing than if you make an awkward assumption and exclude me from anything which involves sharing the Quality Street tin at Christmas.
And if you are going to offer, I like the green triangles best.
Natalie Holborow is an author and poet living in Swansea, Wales
More: Diabulimia - The eating disorder that no one's heard of
More: Chimamanda Ngozi Adichie to Trump defender: As a white man you don't get to define what racism is
Top 100
The Conversation (0)













